Navigating the journey through menopause brings numerous changes to your body, but one of the most visible and frustrating transformations happens right on the surface. Your skin, which has been your protective barrier for decades, suddenly seems to have a mind of its own. Understanding menopause skin disorders becomes essential as hormonal fluctuations create a perfect storm for dermatological challenges that can affect your confidence and comfort. This comprehensive guide explores the specific skin conditions that emerge during this transitional phase and offers practical, natural solutions to help you maintain healthy, radiant skin.
Understanding How Menopause Transforms Your Skin
The relationship between hormones and skin health runs deeper than most people realize.
As estrogen levels decline during perimenopause and menopause, your skin loses its primary support system. Estrogen plays a crucial role in maintaining collagen production, skin thickness, moisture retention, and overall skin barrier function. When these hormone levels drop, menopause affects skin in multiple ways, creating a cascade of changes that manifest as various disorders.
The Hormonal Foundation
Your skin contains estrogen receptors throughout its layers, making it particularly vulnerable to hormonal shifts. These receptors regulate everything from oil production to cellular turnover rates.
Key hormonal changes affecting skin:
- Estrogen decreases by approximately 30% during the first years of menopause
- Progesterone levels drop significantly
- Androgen hormones become proportionally more dominant
- Cortisol sensitivity increases
The imbalance creates conditions where skin becomes thinner, drier, and more reactive to environmental stressors. This foundational shift explains why multiple skin disorders can emerge simultaneously during this phase of life.

Common Menopause Skin Disorders You Might Experience
Menopause skin disorders present in various forms, each with distinct characteristics and triggers.
Severe Dryness and Xerosis
Xerosis, or abnormally dry skin, affects nearly 60% of menopausal women. This condition goes beyond typical dryness, creating tight, flaky skin that may crack or become uncomfortable.
The decline in natural oil production combines with reduced moisture retention capacity. Your skin's lipid barrier weakens, allowing water to escape more readily while environmental irritants penetrate more easily.
Common manifestations:
- Rough, scaly patches on arms and legs
- Tight feeling after cleansing
- Fine lines becoming more pronounced
- Increased sensitivity to weather changes
Natural approaches focusing on barrier repair work exceptionally well for this condition. Look for products containing ceramides, hyaluronic acid, and plant-based oils that mimic your skin's natural lipid composition.
Menopausal Acne and Breakouts
Surprisingly, many women experience acne for the first time during menopause, while others see a resurgence of adolescent patterns.
The proportional increase in androgens stimulates sebaceous glands, particularly along the jawline, chin, and neck. Unlike teenage acne concentrated in the T-zone, hormonal acne typically appears in the lower third of the face and can be stubbornly persistent.
| Teen Acne | Menopausal Acne |
|---|---|
| Forehead and nose focus | Jawline and chin concentration |
| Often responds to topical treatments | May require hormonal consideration |
| Oily skin throughout | Combination: oily chin, dry cheeks |
| Blackheads common | Deeper cystic lesions more frequent |
If you're dealing with combination skin remedies, understanding the hormonal component helps tailor your approach effectively.
Pruritus and Persistent Itching
Menopause itching represents one of the most frustrating symptoms women encounter. This persistent urge to scratch can occur anywhere on the body but commonly affects the arms, legs, and torso.
The mechanism involves multiple factors:
- Decreased estrogen reduces skin hydration
- Natural moisturizing factor (NMF) production declines
- Nerve sensitivity increases
- Inflammatory markers become more active
Some women experience formication, a crawling sensation under the skin, which can be particularly distressing at night. This symptom often disrupts sleep and compounds other menopausal challenges.
Rashes and Increased Sensitivity
Hormonal shifts can lead to skin rashes that appear without clear external triggers. These rashes may present as red, blotchy areas that come and go seemingly at random.
Your skin's barrier function weakens during menopause, making you more susceptible to:
- Contact dermatitis from previously tolerated products
- Photodermatitis and sun sensitivity
- Heat rash during hot flashes
- Allergic reactions to new substances
The connection between hot flashes and skin reactions creates a unique challenge. As your core temperature fluctuates, blood vessels dilate rapidly, sometimes triggering inflammatory responses in sensitive skin.
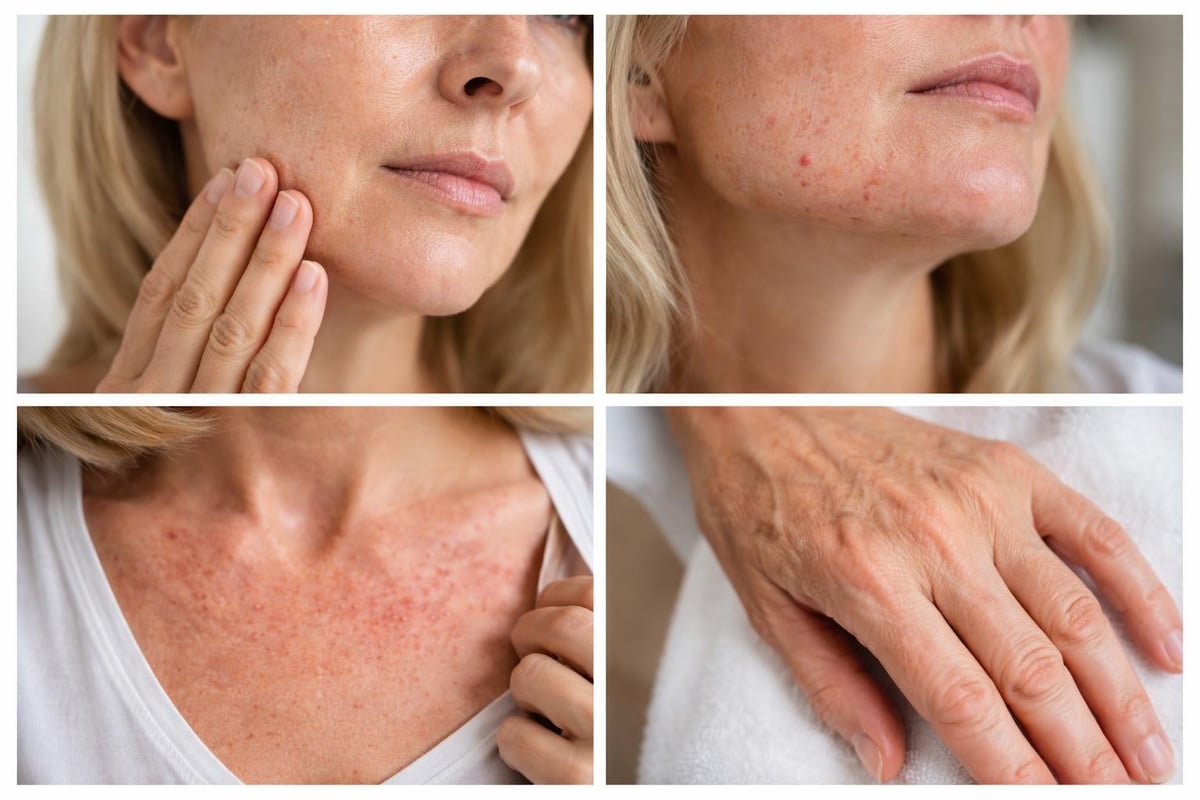
Less Common But Significant Skin Conditions
Beyond the widespread disorders, menopause can trigger specific dermatological conditions that require particular attention.
Keratoderma Climactericum
This rare but distinctive condition affects the palms and soles, causing thickened, sometimes painful skin. Keratoderma climactericum typically develops within the first five years after menopause begins.
The condition manifests as:
- Symmetrical thickening on pressure points
- Yellowish, waxy appearance
- Possible fissuring in severe cases
- Discomfort when walking or gripping objects
While uncommon, recognizing this condition helps distinguish it from fungal infections or psoriasis, ensuring appropriate treatment.
Rosacea Onset or Worsening
Many women experience their first rosacea symptoms during menopause, while those with existing rosacea often see significant worsening.
Triggering factors specific to menopause:
- Hot flashes triggering vascular dilation
- Increased stress and cortisol levels
- Changes in skin barrier function
- Heightened inflammatory responses
The relationship between hot flashes and rosacea creates a challenging cycle. Each hot flash episode can trigger flushing that exacerbates rosacea symptoms, while the anxiety about visible redness may trigger more hot flashes.
Formication and Burning Sensations
Beyond visible changes, some women experience uncomfortable sensory disturbances in their skin. Formication describes the sensation of insects crawling on or under the skin, while burning sensations may occur without visible inflammation.
These neurological symptoms relate to:
- Estrogen's role in nerve function regulation
- Changes in neurotransmitter balance
- Increased nerve sensitivity
- Altered pain perception thresholds
Natural Approaches to Managing Skin Changes
Addressing menopause skin disorders effectively requires a multifaceted approach that works with your changing physiology rather than against it.
Skincare Routine Adjustments
Your tried-and-true products from your 30s and early 40s may no longer serve your evolving needs.
Morning routine essentials:
- Gentle, cream-based cleanser
- Hydrating toner with humectants
- Antioxidant serum
- Rich moisturizer with barrier-repair ingredients
- Broad-spectrum SPF 30 or higher
Evening routine priorities:
- Double cleanse if wearing makeup
- Treatment products for specific concerns
- Retinol or bakuchiol for cell turnover
- Intensive night cream or sleeping mask
The shift toward richer textures and more nourishing formulations reflects your skin's decreased oil production. For those exploring face serums for sensitive skin, choosing formulas with soothing botanicals becomes increasingly important.
Ingredient Selection for Hormonal Skin
Certain ingredients work synergistically with menopausal skin changes, providing targeted support where you need it most.
| Concern | Beneficial Ingredients | How They Help |
|---|---|---|
| Dryness | Hyaluronic acid, Ceramides, Squalane | Restore moisture and barrier function |
| Itching | Colloidal oatmeal, Niacinamide, Centella | Calm inflammation and support healing |
| Acne | Bakuchiol, Salicylic acid, Tea tree | Balance oil without over-drying |
| Sensitivity | Bisabolol, Calendula, Chamomile | Reduce reactivity and soothe irritation |
| Thinning | Peptides, Vitamin C, Retinol | Stimulate collagen and strengthen structure |
Natural formulations often provide gentler alternatives to synthetic actives, particularly important as skin sensitivity increases. Plant-based options like rosehip oil, evening primrose, and sea buckthorn deliver essential fatty acids that support barrier repair.
Lifestyle Modifications That Matter
External care represents only part of the equation. Internal support through lifestyle choices significantly impacts how menopause skin disorders manifest and resolve.
Hydration protocols:
- Drink at least 8-10 glasses of water daily
- Include hydrating foods like cucumber, watermelon, and celery
- Limit dehydrating beverages such as excessive coffee and alcohol
- Use a humidifier in dry environments
Dietary considerations:
- Increase omega-3 fatty acids from fish, flax, and walnuts
- Consume phytoestrogen-rich foods like soy and chickpeas
- Prioritize antioxidant-rich fruits and vegetables
- Consider collagen peptide supplementation
Quality sleep becomes even more critical during menopause, yet often more elusive. Poor sleep exacerbates inflammation, impairs skin repair processes, and intensifies stress responses that worsen skin conditions.
Professional Treatments and Medical Interventions
While natural approaches form the foundation of skin health during menopause, some situations benefit from professional intervention.
When to Consult a Dermatologist
Certain warning signs indicate the need for professional evaluation rather than continued self-treatment.
Seek medical attention for:
- Persistent rashes lasting more than two weeks
- Severe itching interfering with sleep or daily activities
- Sudden changes in existing moles or skin lesions
- Painful cystic acne not responding to over-the-counter treatments
- Signs of infection such as oozing, fever, or spreading redness
Clinical reviews of skin disorders during menopause emphasize the importance of proper diagnosis, as some conditions require prescription treatments for effective management.
Hormone Replacement Therapy Considerations
For some women, systemic hormone replacement therapy (HRT) can significantly improve skin health alongside other menopausal symptoms.
Research shows that estrogen therapy can:
- Increase skin collagen content by 30% or more
- Improve skin thickness and elasticity
- Enhance moisture retention capacity
- Reduce the severity of menopausal acne
However, HRT isn't appropriate for everyone. Discuss your complete medical history with your healthcare provider to determine if this option aligns with your individual health profile and risk factors.
Topical Prescription Options
Dermatologists can prescribe targeted treatments for specific menopause skin disorders that don't respond adequately to over-the-counter solutions.
Common prescription approaches:
- Topical estrogen creams for localized dryness (used cautiously)
- Prescription retinoids for acne and anti-aging
- Corticosteroid creams for inflammatory rashes (short-term use)
- Prescription-strength moisturizers for severe xerosis
These treatments work best when combined with appropriate natural skincare routines and lifestyle modifications.

Building Your Personalized Care Strategy
No single approach works for everyone experiencing menopause skin disorders. Your unique skin history, genetics, and overall health status all influence which strategies will serve you best.
Assessment and Tracking
Start by honestly evaluating your current skin status and tracking changes over time.
Create a skin journal documenting:
- Specific symptoms and their severity (scale of 1-10)
- Products currently in use
- Dietary patterns and water intake
- Sleep quality and stress levels
- Correlation with menstrual cycle (if still present)
This systematic approach helps identify patterns and triggers while providing valuable information if you eventually consult a dermatologist.
Gradual Product Transitions
Resist the urge to overhaul your entire routine overnight. Your skin needs time to adjust to new formulations, especially during this sensitive transition period.
Introduce new products one at a time, waiting at least two weeks before adding another. This methodical approach helps identify any ingredients that trigger reactions and prevents overwhelming your compromised skin barrier.
When exploring natural face creams, start with patch testing on a small area before full-face application. Your skin's reactivity may surprise you, even with products you've used successfully in the past.
The Role of Stress Management
Chronic stress significantly exacerbates menopause skin disorders through multiple mechanisms. Elevated cortisol levels impair skin barrier function, increase inflammation, and slow healing processes.
Effective stress reduction techniques:
- Daily meditation or mindfulness practice (even 10 minutes helps)
- Regular moderate exercise (walking, swimming, yoga)
- Adequate sleep prioritization (7-9 hours nightly)
- Social connection and community support
- Professional counseling when needed
The mind-skin connection operates powerfully during menopause. Women who actively manage stress often see more dramatic improvements in skin health than those focusing solely on topical treatments.
Special Considerations for Different Skin Types
Your baseline skin type influences how menopause skin disorders manifest and which treatments work best.
Previously Oily Skin
If you've spent decades battling excess oil, menopause may actually normalize your sebum production. However, the transition can create confusion as your skin sends mixed signals.
You might notice:
- Oily T-zone with dry cheeks developing
- Need for lighter moisturizers than expected
- Continued breakouts despite reduced overall oiliness
- Better tolerance for active ingredients previously too harsh
Adjust your routine gradually, incorporating more hydration while maintaining oil control where needed. You may find yourself appreciating combination skin remedies for the first time.
Previously Dry Skin
Women with inherently dry skin often experience the most dramatic changes during menopause. The existing moisture deficit compounds with hormonal decreases, creating severely compromised barrier function.
Intensive care strategies:
- Layer multiple hydrating products (essence, serum, cream)
- Use occlusive ingredients like shea butter and oils at night
- Minimize cleansing to once daily
- Avoid hot water and harsh cleansers completely
- Consider facial oils as your primary moisturizer
Your skin may require richer formulations than you ever imagined using. Embrace these nourishing textures as tools for maintaining comfort and health.
Sensitive and Reactive Skin
If your skin has always been particular, menopause amplifies these tendencies. The decreased barrier function makes previously tolerated ingredients suddenly problematic.
Simplify ruthlessly. Strip your routine to absolute essentials, focusing on gentle cleansing and intensive moisturizing. Add back actives only after establishing a stable baseline.
Prevention and Long-Term Skin Health
While you can't prevent menopause itself, proactive measures significantly influence how severely skin disorders develop and persist.
Sun Protection as Foundation
UV damage accumulates over decades, but the thinning skin of menopause makes existing damage more visible while increasing vulnerability to future harm.
Non-negotiable sun protection rules:
- Apply SPF 30+ daily, even indoors (UVA penetrates windows)
- Reapply every two hours when outdoors
- Seek shade during peak UV hours (10 AM to 4 PM)
- Wear protective clothing, hats, and sunglasses
- Don't rely on makeup SPF as your only protection
The relationship between sun exposure and accelerated aging intensifies during menopause. Research on skin disorders during menopause confirms that UV protection becomes even more critical during this transition.
Nutrition for Skin Support
What you eat directly impacts your skin's ability to maintain health during hormonal upheaval.
Skin-supporting nutrients:
- Vitamin C for collagen synthesis (citrus, berries, peppers)
- Vitamin E for antioxidant protection (nuts, seeds, avocado)
- Omega-3 fatty acids for inflammation control (fatty fish, flax)
- Zinc for healing and oil regulation (pumpkin seeds, chickpeas)
- Biotin for overall skin health (eggs, sweet potatoes, almonds)
Consider working with a nutritionist to develop an eating plan that supports skin health alongside overall menopausal wellness. The synergy between internal nutrition and external care creates the most dramatic improvements.
Regular Professional Monitoring
Annual skin examinations with a dermatologist help catch concerning changes early while providing expert guidance on managing evolving conditions.
As you navigate these changes, remember that menopause skin disorders represent a normal physiological response to hormonal shifts, not a personal failing. With patience, appropriate care, and self-compassion, you can maintain healthy, comfortable skin throughout this transition and beyond.
Managing menopause skin disorders requires understanding the hormonal foundation driving these changes and implementing targeted natural solutions that support your skin's evolving needs. By combining appropriate skincare products, lifestyle modifications, and professional guidance when needed, you can navigate this transition with confidence and maintain the healthy, radiant skin you deserve. Sinusoothe Ltd offers carefully formulated natural skincare products designed to address the specific challenges of hormonal skin changes, providing gentle yet effective support during menopause and beyond.







